
Outsourced Medical Billing Services You Can Trust
The visibility, effort, and team approach you need to collect more revenue.

Trusted by today’s leading healthcare organizations
|
|
 |
 |
 |

Streamline Your Billing with AI
Simplify your revenue cycle with the ADSRCM AI Rules Engine, designed to improve claim accuracy, speed up reimbursements, and enhance your financial performance.
- Streamlined Claims Process: AI ensures clean and compliant claims for faster payments.
- Reduced Errors: Advanced technology catches mistakes before they happen.
- Increased Efficiency: Minimize paperwork and administrative tasks for your team.
90%
of medical practices say costs have
risen faster than revenues.*
58%
of medical practices say staffing
is their biggest challenge.*
56%
of medical groups say time in A/R
increased in 2022.*
We address every step in the patient process to improve your revenue capture
Every step in the patient process is optimized to maximize your revenue capture.
Credentialing
Registration
Prior Authorization and Eligibility
Charge Entry and Coding Review
Claim Scrubbing and Submission
Automated Denial and Appeals Management
Payment Posting and Patient Collections
Weekly Performance Review
Building a KPI mindset for growth
Key industry metrics such as these and process improvement strategies will help drive your revenue cycle.
98%
Authorization Capture
99%
Clean Claim Rate
(First Pass)
98%
Verified Insurance Eligibility Success
< 48
Hour Claim Submission
< 5%
Denial Rate
< 30
Target A/R Days
90%
Collections within
90 Days
96%
Collections within 120 Days
< 30%
Self Pay A/R
< 3%
Bad Debt

Data-driven medical billing services
Our 300+ outsourced billing team helps alleviate staffing issues and reduce operating costs by consolidating in-house resources for maximized efficiency.
You'll get insight and clarity on your billing and collections processes including:
- regularly scheduled financial meetings to review your key performance metrics and your practice’s overall financial health
- reviewing outstanding A/R and expected future revenue
- real-time financial KPI dashboards and analytics
- recommending process improvements to drive claims processing and patient payments

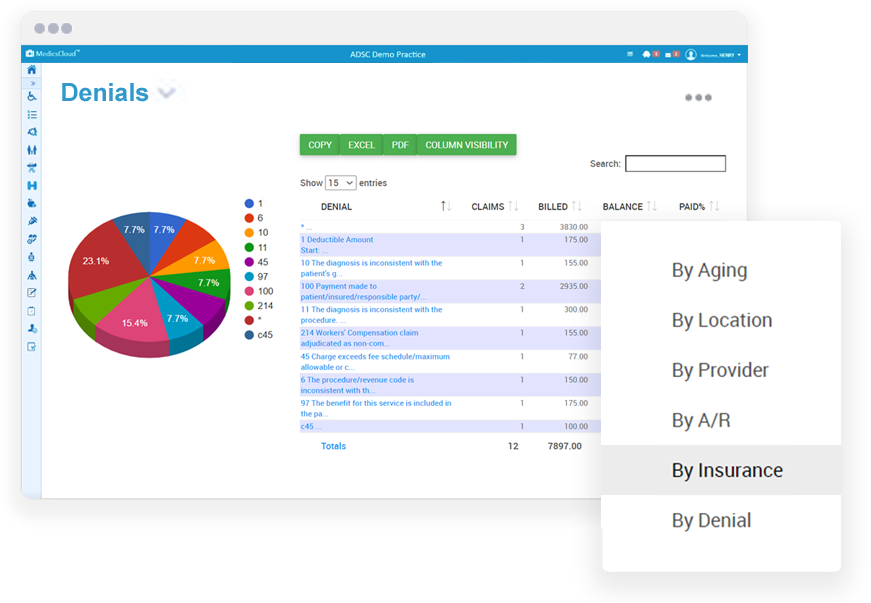
Maximize your claims
We know your payer mix, your state billing requirements, and your specialty.
- Claims are submitted at their highest possible value
- Out-of-network alerts on scheduling
- Automated eligibility verification and insurance discovery
- Proactive denial management

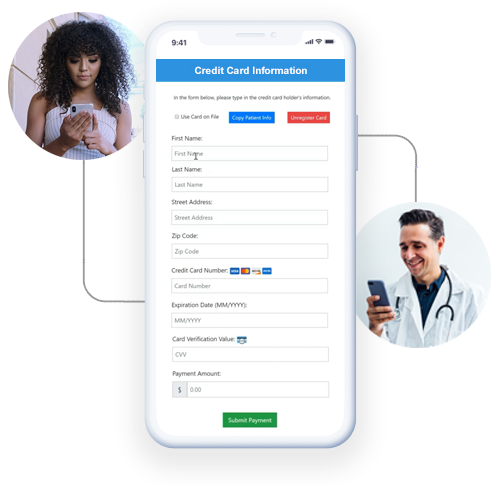
Capture patient balances
Use an array of features that work to reduce your outstanding patient balance A/R:
- Access to a patient responsibility estimator
- Enabling patients to pay from any mobile device
- Interactive balance due reminder texting

Comply with complicated CMS initiatives
We stay ahead of the seemingly never-ending billing regulations affecting your practice including:
- No-Surprises Act
- Cures Act
- Clinical decision support
- MIPS reporting


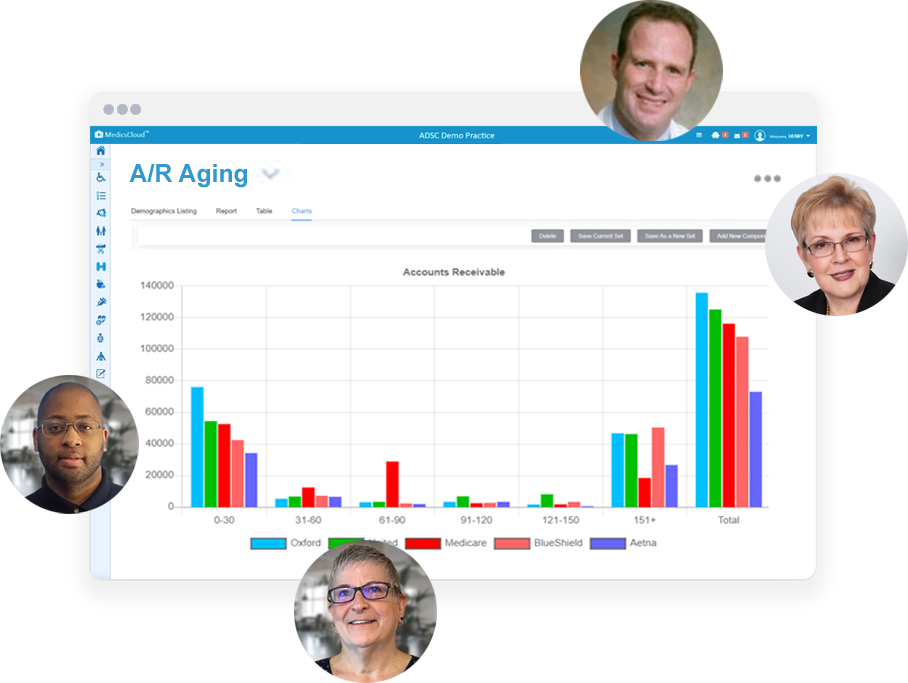
Understanding your revenue
Following MGMA financial reporting recommendations, MedicsRCM produces comprehensive financial and management reports, analytics and KPIs.
- Benchmarking metrics
- Key Performance Indicator (KPI) metrics
- Best practices for billing

What our customers are saying
"During this extremely difficult (COVID-19) time we could NOT have asked for a better business partner than MedicsRCM to handle our EHR and billing. The MedicsRCM team has been truly amazing in helping to retain revenue to keep our business running, and to be there for our patients."
Charles Saha, MD | Park Avenue Medical Professionals
"Working with MedicsRCM has proven to be a very professional experience for my staff, giving them the ability to turn to a single source, and to get any questions quickly answered. Most importantly, reimbursements have gone up! Overall, MedicsRCM has made the practice so much better."
Thomas Beggins, MD | Connecticut Eye Physicians PC
Put our experience to work for you
Our management team has over 200 combined years of experience in RCM and billing services.

Sheryl Miller, MBA
EVP of Sales & BD, RCM Services

Gene Spirito, MBA
National Sales Manager, RCM
.png?width=231&height=170&name=Jim-ONeill-Lab%20(1).png)
Jim O'Neill
Sales Manager, Laboratory RCM
.png?width=231&height=170&name=Scott-Friedman-BH%20(1).png)
Scott Friedman
Director of Sales, RCM Division

Marybeth McGowen
RCM Division Manager

Daphna Barzillai, MBA
RCM A/R Manager

Vishal Upraity
Associate Director - RCM

Kim Becker
National Portfolio Manager
Outsourced Medical Billing Services FAQs
We know selecting an outsourced medical billing company can be difficult. You probably have loads of questions, so let’s get you started on some of the most frequently asked questions we get.
What does your outsourced medical billing service cost?
MedicsRCM pricing is based on a percentage of the amount collected for you, with percentages generally ranging from 3% to 6% based on the collection amount.
How long does it take to transition to your medical billing service?
We can start to submit your claims in as little as 30 days once our 5-7 days of testing is completed.
Will I have single or multiple points of contact with your medical billing service?
A MedicsRCM Services Manager, experienced in your specialty(ies), is assigned under whom following resources operate:
- Dedicated Account Manager
- Billing Team Members
- EDI specialists for claims, remittances, EOB reconciliations, eligibility verifications, and direct fund deposits
- HL-7 interface specialist
- A senior member of the ADS management team is also connected with each MedicsRCM client
How will my current databases be handled?
We import your current files such as Referring Physician, Insurance, and Fees into our MedicsPremier practice management system.
What system does your medical billing service use?
MedicsRCM uses the MedicsPremier system which is our own product, relied on by tens of thousands of medical practices to process tens of millions of EDI transactions annually. Something traditional outsourced medical billing servers can't offer. Our clients benefit in how we don’t rely on a second or third party software vendor for support and updates. ADS has been a leading medical software company since 1977.
Does your medical billing service start sending our claims from Day One?
No one wants to submit all of your claims more than we do since we only get paid on amounts collected. But, that would be irresponsible. Instead, we submit test claims for 50 to 100 of your patients for approximately 5 to 7 days. All of your claims are submitted once the test claims are verified.
What happens if my current billing company stops submitting our claims?
We can bill and resubmit those claims. In fact, MedicsRCM tracks old claims vs. new claims.
Do we have access to our data?
Yes, MedicsRCM clients have 24 x 7 on-demand cloud access to all of their data. We train clients on using our MedicsPremier system, and encourage them to see how things are going!
What if we need customized management reports?
Clients almost never need truly customized reports since our reports/dashboards as so highly user-defined, and are exportable to Excel. But if a certain customized report(s) are needed, your Accounts Team will provide same via standard PDF or Excel.
Are forms needed for electronic claims?
Possibly, and if so, we provide you with whatever form(s) are needed by any insurance payer(s) and provide assistance, if needed, in completing them. Of course 100% electronic claims and EOB reconciliations - which our team handles for you - are encouraged.
What about patient responsibility balances?
First, clients have access to our patient responsibility estimator, a powerful feature for obtaining personal balances. MedicsRCM processes patient statements. Patients are directed to call us, not you, with statement questions. Our portal has an option for online credit card payments, and our balance due texting option is ideal for reminding patients about what they owe. Texts can link to the portal for patients to make their payments online. Texting is also excellent for reminding patients about their appointments.
Can your medical billing service help if patients don’t have insurance?
Yes! Our insurance discovery option has a very high rate of success in identifying patients’ insurance when it’s missing or unavailable.
Does your medical billing service have any tools for mobility and engagement?
Yes, with our options for Medics Telemedicine, Portal, Texting, Kiosk for expedited intake, and even for remote patient monitoring (RPM) of vitals. Telemedicine and RPM are ideal for generating revenue and texting keeps patients tuned into their in-office and telemedicine appointments while helping to eliminate no-shows.
Can we use an EHR with your medical billing service?
We actually have three options for EHR! One is to use our certified MedicsCloud EHR which is excellent for any number of specialties. Or, you can keep your existing EHR with an interface to our MedicsPremier system. Our third option is our Medics e-superbill if you prefer to not use an EHR or to have your existing EHR interfaced with us. Either way, we have your medical practice covered.
Keep up with the lates billing trends, insights, and industry news
Medical Billing / RCM
The Difference Between Professional Billing and Facility Billing for Inpatient Care
A patient is admitted for a major procedure. The surgeon performs the operation. The ...
By Gene Spirito, MBA
on June 4th, 2026
Medical Billing / RCM
Observation Status vs Inpatient Admission: The Billing Difference That Costs Patients Thousands
A patient spends four nights in the hospital after cardiac symptoms. They feel cared for. The ...
By Gene Spirito, MBA
on June 3rd, 2026
Medical Billing / RCM | RCM | Orthopedic
Orthopedic RCM Software vs Full-Service RCM: Which Does Your Practice Need?
Your orthopedic billing team is stretched. Denials are up, AR is aging, and your billers are ...
By Adam Andrew
on May 28th, 2026