Accelerate your workflow with intelligent practice management software
Automate scheduling, reduce claim errors, and simplify daily tasks—so your team can move faster and focus on care.

Trusted by today’s leading healthcare organizations







The practice management software that gets you paid more
“We value how the system really does help us capture every maximized dollar for every patient visit. MedicsPremier has produced an incalculable return on investment.”
Rory Hansen, Practice Administrator | Park Avenue Medical Associates
“We value how the system really does help us capture every maximized dollar for every patient visit. MedicsPremier has produced an incalculable return on investment.”
Rory Hansen, Practice Administrator | Park Avenue Medical Associates
“MedicsPremier allows us to capture every dollar for every visit which helps us operate at peak efficiency.”
Karrie deMas, Billing Manager | Thorp Bailey Weber Eye Associates
“MedicsPremier allows us to capture every dollar for every visit which helps us operate at peak efficiency.”
Karrie deMas, Billing Manager | Thorp Bailey Weber Eye Associates
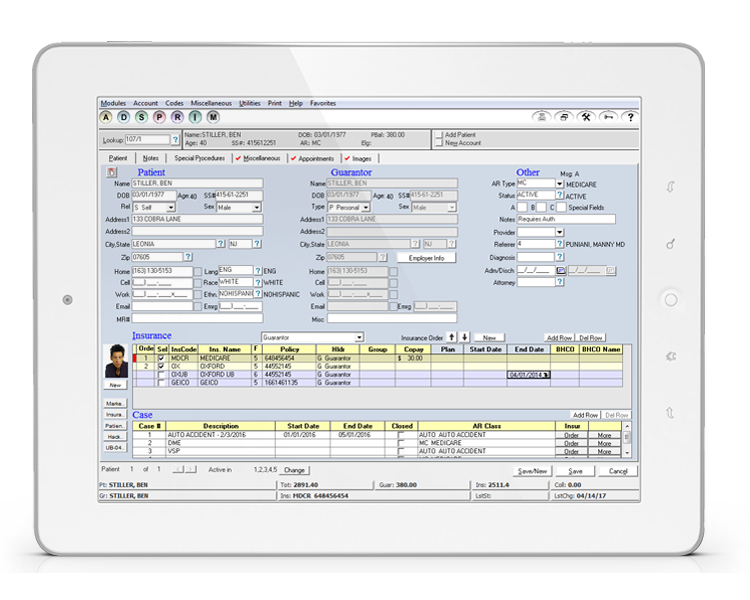
Protect revenue before the visit
Catch denials early and set payment expectations before the patient arrives.
- Out-of-network alerts during scheduling
- Patient responsibility estimator at check-in
- Automated copay reminders
- Batch eligibility checks
- Denial risk alerts before claims go out

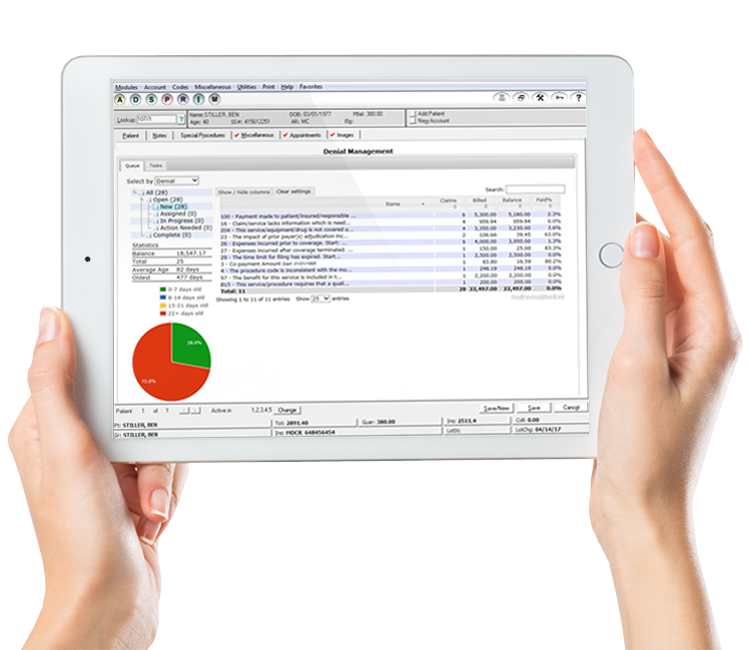
Get paid on the first try
Submit clean claims and keep rework to a minimum with built-in claim intelligence.
- Near-perfect first-attempt clearinghouse success
- Supports HCFA, UB, Workers’ Comp & No-Fault
- Over-coding alerts to optimize reimbursements
- Real-time claim tracking and editing
- Hands-off follow-up with secondary insurers

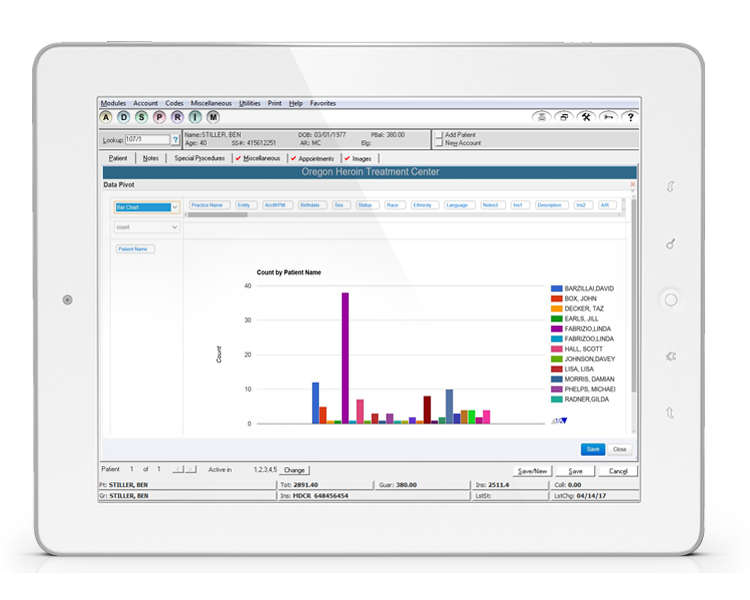
Sell services without the hassle
Manage products, payments, and non-medical visits—right alongside medical appointments.
- Inventory and sales tax tracking
- Accept gift cards, coupons, cards, and checks
- Schedule and report on non-medical visits
- Separate financial reporting by service type
- All-in-one scheduling for medical and non-medical

Make patient payments simple
Encourage real-time payments and reduce aging A/R before patients even leave.
- Show balances owed after insurance
- Request partial or full payments on the spot
- Auto-generate and send statements
- Text reminders for outstanding balances
- Secure online payments via patient portal

Features built to boost productivity
Advanced Scheduler
The multi-modality Scheduler is a robust financial system. Schedule staff, resources, and ancillary services related to the appointment in any type of medical practice.

Text Reminders
Medics SMS™ for interactive text reminders to patients’ cellphones about upcoming appointments. Patients reply with a confirmation or a request to cancel.
Information Management
Comprehensive, extremely intuitive demographics panel; commonly-needed demographics data is displayed on virtually every system view.
Separate Tax IDs
The Suite accommodates a single, or an unlimited number of tax IDs while its built-in MPI architecture ensures identifying the correct patient for your medical practice.
CRM for Marketing
Use the built-in CRM features to track marketing/advertising campaigns, or integrate with almost any other CRM or management software.
Analytics and KPIs
Our practice management software offers detailed financial and operational reports, with KPIs displayed in dashboards, and most reports can be exported to Excel.
Make your Statement
Create clear patient statements, produce them offsite cost-effectively, and send balance reminders via text.
Mobile App
The MedicsMobile™ option gives providers the ability to connect using almost any smartphone or internet-enabled device.
Integrated Certified EHR
Use our own certified MedicsCloud EHR, or yours interfaced with MedicsPremier, or no EHR with our e-superbill.
Keep up with the latest practice management software trends, insights, and industry news
Practice Management | KPI
5 KPIs Every Practice Administrator Should Be Tracking in 2026
You know the feeling. The end of the month arrives, the reports run, and somewhere in a spreadsheet ...
By Gene Spirito, MBA
on April 30th, 2026
Medical Billing / RCM | Practice Management | EMR
Ten Drudgeries You Don’t Need To Do Anymore
There are two types of drudgeries:
By Marc Klar
on June 13th, 2025
Medical Billing / RCM | Practice Management
Can RCM Software Help Your Medical Practice Stop Losing Revenue?
If your medical practice is leaving revenue on the table because of inefficient billing and ...
By Christina Rosario
on May 16th, 2025

